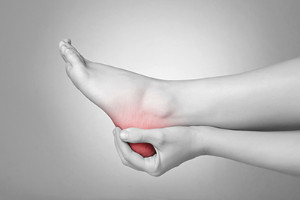
 Plantar fasciitis is the result of the plantar fascia, the band on the bottom of the foot that connects the toes to the heel, becoming inflamed. Plantar fasciitis usually results in pain at the bottom of the heel or midfoot. Generally, the pain develops over time and can be either sharp or dull. Pain from plantar fasciitis is usually worse after waking up in the morning, after sitting or lying down for a long period of time, or after climbing stairs. Pain from plantar fasciitis is usually felt after an activity is completed and not as much during the activity. People who are between the ages of 40 and 70 and are active are at a higher risk of developing plantar fasciitis. Those who are obese, pregnant, run long distances, have structural foot problems, or have a very active job are also at a higher risk of developing plantar fasciitis. If you are experiencing the symptoms of plantar fasciitis, it is important to visit a podiatrist for a proper diagnosis and treatment plan.
Plantar fasciitis is the result of the plantar fascia, the band on the bottom of the foot that connects the toes to the heel, becoming inflamed. Plantar fasciitis usually results in pain at the bottom of the heel or midfoot. Generally, the pain develops over time and can be either sharp or dull. Pain from plantar fasciitis is usually worse after waking up in the morning, after sitting or lying down for a long period of time, or after climbing stairs. Pain from plantar fasciitis is usually felt after an activity is completed and not as much during the activity. People who are between the ages of 40 and 70 and are active are at a higher risk of developing plantar fasciitis. Those who are obese, pregnant, run long distances, have structural foot problems, or have a very active job are also at a higher risk of developing plantar fasciitis. If you are experiencing the symptoms of plantar fasciitis, it is important to visit a podiatrist for a proper diagnosis and treatment plan.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
 Excess levels of uric acid in the blood may lead to the medical condition that is known as gout. Crystals can form in the joints of the big toe, and this can cause severe pain and discomfort. Additional symptoms that patients experience may consist of swelling, heat and redness, and it may become difficult to walk. Gout is considered to be a form of arthritis and it can develop for a variety of reasons. These can include genetic factors, eating foods that have high purine levels, or from taking certain medications. When a gout attack occurs it can be beneficial to rest and elevate the affected foot, as well as apply ice packs and take anti-inflammatory medication, and the pain may be reduced. Gout can be a debilitating foot condition, which is why you should consult with a podiatrist as quickly as possible so correct treatment options can be discussed.
Excess levels of uric acid in the blood may lead to the medical condition that is known as gout. Crystals can form in the joints of the big toe, and this can cause severe pain and discomfort. Additional symptoms that patients experience may consist of swelling, heat and redness, and it may become difficult to walk. Gout is considered to be a form of arthritis and it can develop for a variety of reasons. These can include genetic factors, eating foods that have high purine levels, or from taking certain medications. When a gout attack occurs it can be beneficial to rest and elevate the affected foot, as well as apply ice packs and take anti-inflammatory medication, and the pain may be reduced. Gout can be a debilitating foot condition, which is why you should consult with a podiatrist as quickly as possible so correct treatment options can be discussed.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
Risk Factors
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout is a form of arthritis that is caused by a buildup of uric acid crystals in the joints. This considered to be one of the most frequently recorded medical illnesses throughout history. Gout occurrences in the US have risen within the past twenty years and the condition now affects 8.3 million people which is 4% of all Americans. Researchers have found that gout affects men more than women and African-American men more than white men.
Symptoms of gout are warmth, swelling, discoloration, and tenderness in the affected joint area. The small joint on the big toe is the most common place for a gout attack to occur.
People who are obese, gain weight excessively, drink alcohol heavily, have high blood pressure, or have abnormal kidney function are more likely to develop gout. Furthermore, certain drugs and diseases are likely to increase levels of uric acid in the joints which eventually leads to gout. You are also more likely to develop gout if you eat a lot of meat and fish.
Many who experience gout attacks will experience repeated attacks over the years. Some people who have gout symptoms, may never have them again, but others may experience them several times a year. If you have gout symptoms throughout the year, you may have recurrent gout. Those who have gout should also be careful about their urate crystals collecting in their urinary tract, because this may lead to kidney stones.
Diagnosis for gout is done by checking the level of uric acid in the joints and blood. Your podiatrist may also prescribe medicine to reduce uric acid buildup in the blood, which will help prevent any gout attacks.
To treat gout, your podiatrist may also prescribe you Anti-inflammatory medication (NSAIDs) which will relieve the pain and swelling of a gout episode and it can also shorten a gout attack. Maintaining a healthy diet is also a proven method to prevent gout attacks.
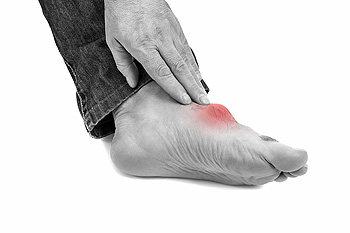
 The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
The tibial nerve is located in a small tunnel surrounded by tendons in the inner side of the ankle. Tarsal tunnel syndrome can develop when this specific nerve becomes compressed, and is often accompanied by pain and swelling. It may happen as a result of enduring an ankle injury, such as a sprain or fracture, or from having bone spurs. Mild relief may be found when the affected foot is elevated, and it may help to take anti-inflammatory medication. In severe cases, surgery can be a viable option to permanently reduce or eliminate the pain that is associated with this condition. If you have developed this ailment, it is strongly recommended that you speak with a podiatrist who can help you choose the correct treatment option.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Brian Shwer, DPM of Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
The Effects of Tarsal Tunnel Syndrome
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tarsal tunnel syndrome is a condition in which the tibial nerve, located in the tarsal tunnel in the foot, is compressed. The tibial nerve can become compressed from injury, such as an ankle sprain, flat feet, and lesions. Arthritis, diabetes, and varicose veins can also cause swelling and thus result in nerve compression.
Symptoms of tarsal tunnel syndrome include several different sensations in the sole of the foot, inside the ankle, and around the tibial nerve. These sensations include shooting pains, numbness or reduced sensation, pins and needles, burning, and tingling. Symptoms tend to worsen with greater activity to the area. In rare and severe occasions, this can change the muscles in the foot.
If you suspect you have tarsal tunnel syndrome, you should consult with your podiatrist. He or she will examine your medical history to see if you have a history of diabetes, arthritis, or flat feet. They will also check to see if you have suffered an injury to the area recently. An electrical test will be conducted to check if the nerve has been damaged. A simpler Tinel’s Test might also be used. This includes simply tapping the nerve to create a sensation. An MRI scan of the area may also be used.
Treatments vary greatly for tarsal tunnel syndrome. Treatments include both nonsurgical and surgical options depending upon the severity of the condition. Nonsurgical options include anti-inflammatory medication and steroid injections to the area. Orthotics, such as a splint or brace that immobilizes the foot, is another noninvasive option. For those with flat feet, custom shoes can be made to offer better foot support. Surgical options include a tunnel tarsal release, in which an incision is made behind the ankle down to the arch of the foot. This releases the ligament and relieves pressure off the nerve. Some doctors use a more minimally invasive surgery, where smaller incisions are made in the ankle and the ligament is stretched out.
If you are suffering from painful sensations in your foot, see a podiatrist who can determine if you are experiencing tarsal tunnel syndrome. Tarsal tunnel syndrome that is left unchecked can cause permanent nerve damage to the foot.
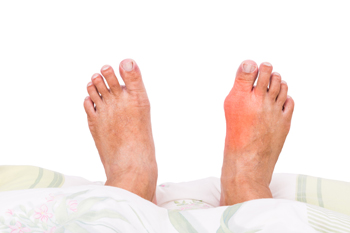 A bunion is a bony bump that forms along the base of the big toe. Bunions can cause pain and stiffness in the affected foot, as well as swelling. Sometimes surgery, also known as a bunionectomy, may be necessary to correct the deformity and relieve the pain. You may consider bunion surgery if you have severe pain when walking, even when you’re wearing flat comfortable shoes, or when you are unable to bend or straighten the big toe. Other reasons to consider surgery can be chronic inflammation of the big toe that doesn’t go away with rest or medicine, if the big toe becomes deformed, or if the big toe bends towards the smaller toes. A podiatrist can evaluate the severity of your bunion and determine if surgery is the correct method of treatment for you.
A bunion is a bony bump that forms along the base of the big toe. Bunions can cause pain and stiffness in the affected foot, as well as swelling. Sometimes surgery, also known as a bunionectomy, may be necessary to correct the deformity and relieve the pain. You may consider bunion surgery if you have severe pain when walking, even when you’re wearing flat comfortable shoes, or when you are unable to bend or straighten the big toe. Other reasons to consider surgery can be chronic inflammation of the big toe that doesn’t go away with rest or medicine, if the big toe becomes deformed, or if the big toe bends towards the smaller toes. A podiatrist can evaluate the severity of your bunion and determine if surgery is the correct method of treatment for you.
If you are suffering from bunions, contact Brian Shwer, DPM of Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.