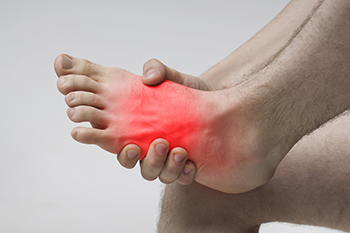
Dancers and basketball players, as well as runners, may be familiar with stress fractures in the feet. This overuse injury, which consists of hairline fractures of the bones in the foot, often results from repetitive pounding on hard surfaces. A sudden increase in activity, such as playing longer and more often, or adding excess mileage to a run, can result in developing stress fractures. These tiny cracks are easy to dismiss at first because the pain often diminishes with rest. They also are difficult to detect with a foot X-ray, and often may only be noticed through digital imaging tests. Certain types of footwear, exercise equipment and surfaces, as well as insufficient rest periods are other major contributors to foot stress fractures. Finally, osteoporosis, arthritis, and neuropathy can be factors. A podiatrist can offer a clear diagnosis of stress fractures, and depending on the severity can offer the appropriate treatment options. For more information, it is suggested that you make an appointment with a podiatrist.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
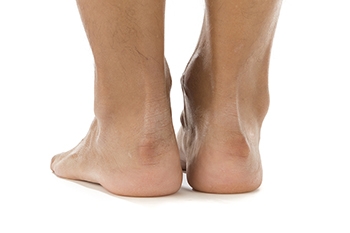
Haglund's deformity is a foot abnormality where the heel bone and soft tissues develop an enlarged bony section at the Achilles insertion, causing heel pain and swelling. It is linked to retrocalcaneal bursitis, often referred to as "pump bump" or "winter heel" due to pressure from pump-style shoes. This condition commonly affects runners and women aged 15 to 35, particularly those who wear high heels. Factors such as genetics, high arches, tight Achilles tendon, and walking on the outer heel edge contribute to its formation. Wearing tight or ill-fitting shoes also exacerbates the condition. Treatment ranges from anti-inflammatories to surgery to remove the bony protrusion. If you have a bump on the back of your heel that causes foot pain, it is suggested that you consult a podiatrist for an accurate diagnosis and appropriate treatment.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Southaven, MS . We offer the latest in diagnostic and treatment technology to meet your needs.
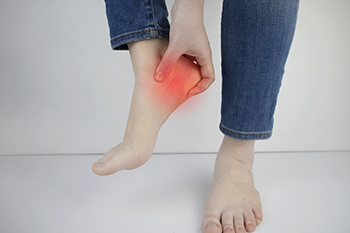
A band of tissue called the plantar fascia runs along the sole of the foot, connecting the toes to the heel. When this tissue becomes inflamed, it can result in pain in the foot, arch, and heel, and is a condition termed plantar fasciitis. Although the plantar fascia is built to absorb pressure, if too much is applied, the plantar fascia can tear. It is a common condition among walkers, runners, and other athletes, and is the most frequent complaint of heel pain. Symptoms can include a sharp or burning pain in the heel that feels worse when you get up in the morning but wears off after activity begins. Plantar fasciitis also can make lifting the toes off the ground more difficult. If the pain inhibits performing normal daily activities, or if it stops you from sleeping, it may be time to get medical help. Ignoring plantar fasciitis can lead to long-term heel pain. An X-ray or additional imaging tests can help to determine the cause and severity of the heel pain. If you think you may have plantar fasciitis, it is suggested that you make an appointment with a podiatrist who is trained to deal with this condition.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
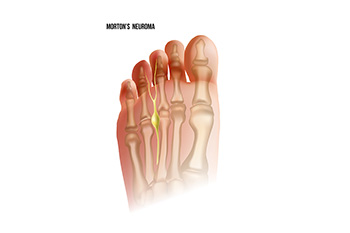
Foot pain is a common ailment. It can happen in different areas of the foot and for various reasons. Pain that occurs between the third and fourth toes may indicate Morton’s neuroma has developed. It is a condition that affects the nerve between these toes and causes it to become compressed and irritated. Morton’s neuroma is generally caused by wearing shoes that do not have enough room in the toe area, such as high heels. It is beneficial to choose a shoe with a wider toe box if high heels are desired to be worn. Common symptoms that are associated with Morton’s neuroma can consist of a burning or tingling sensation, and many people feel as if there is a small pebble in their shoe or sock. Relief may be found in the beginning stages of Morton’s neuroma by wearing shoes that fit correctly. For progressed cases, it may be necessary for a more invasive treatment to be performed. If you have pain in this part of your foot, it is suggested that you seek the counsel of a podiatrist who can effectively diagnose and offer correct treatment options for Morton’s neuroma.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Brian Shwer, DPM of Southaven Foot Clinic. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
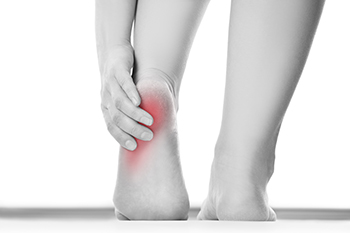
Heel pain is a common foot condition, and there are various reasons why it can happen. The largest tendon in the body is called the Achilles tendon, and it attaches to the heel. An injury can cause this tendon to become torn or irritated, and heel pain may ensue. Many people suffer from plantar fasciitis, which is caused by an inflamed plantar fascia. This is the band of tissue that connects the heel to the toes, and the pain is often felt in the heel. The condition that is known as neuropathy can cause the inability to feel sensations in the foot, including the heel. Waking can be difficult, and patients may need to use a cane or walker to maintain balance. A stone bruise is a heel disorder that can happen to people who jump from heights and lands on their feet. This condition may affect the heel pad, which acts as a shock absorber and may possibly become damaged. If you have heel pain, it is strongly suggested that you confer with a podiatrist who can determine what the reason is and offer treatment options that are correct for you.
Many people suffer from bouts of heel pain. For more information, contact Brian Shwer, DPM of Southaven Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
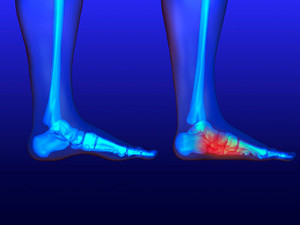
The foot condition that is referred to as flat feet indicates the foot has no arch, or it may be very low. The majority of babies are born with flat feet, which may extend into adulthood as a result of genetics or enduring a foot injury. There are some patients who experience pain with flat feet, and their posture may be affected. People who have flat feet and enjoy running may have to learn specific stretches that can help to strengthen the overall foot before embarking on a run. It is beneficial to stretch the foot before and after every run. This can be done by placing the foot on top of a golf ball and rolling back and forth several times. The Achilles tendon can be stretched by performing appropriate calf stretches. It is beneficial to wear running shoes that are designed for people who have flat feet. These types of shoes may provide adequate arch support in addition to stability, support, and comfort. If you have flat feet and love to run, it is strongly suggested that you confer with a podiatrist who can provide you with information that can protect your feet while running.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Brian Shwer, DPM from Southaven Foot Clinic. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
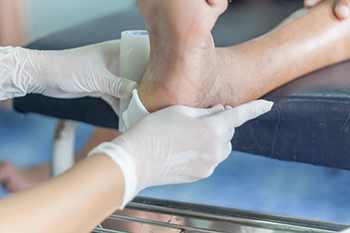
As the summer months begin, the risks of cutting or otherwise wounding your feet may increase. Wearing sandals or flip flops, as well as going barefoot more often can increase the chances of having to deal with foot wounds. If you are bleeding profusely from a wound, immediate medical attention is vital. There also may be times when a podiatrist is needed to attend to foot wounds, including punctures, lacerations, toenail injuries, and broken toes. When you step on a nail or other sharp object, the puncture wound may appear small and may not bleed very much. But because the depth of the wound can be a source of infection as well as damage to nerves and tendons, attention from this foot doctor is suggested. Abrasions or scrapes may bleed and ooze fluids, making it difficult to clear it from debris. To avoid infection setting in, it is suggested that you make an appointment with a podiatrist. Similarly, if you have a skin injury and have diabetes or vascular disease, seeing a podiatrist as soon as possible is strongly suggested.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Brian Shwer, DPM from Southaven Foot Clinic. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot care needs.
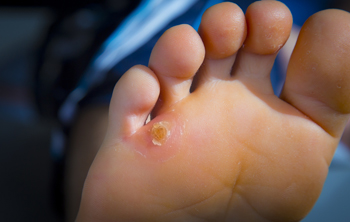
Corns are thickened areas of skin that can develop on feet and toes. They are caused by prolonged pressure or friction and can happen from shoes that do not fit well, and performing repetitive activities. Additionally, foot conditions with deformities that press against shoes, such as bunions or hammertoe may cause corns to develop. A seed corn, or heloma millare, is one of three types of foot corns, and can also occur from having dry skin. They are small and can appear on the soles of the feet. It may be difficult to distinguish them from calluses or plantar warts, and a sample will have to be taken for examination under a microscope. Seed corns are hard, circular, and have well-defined spots on the skin and are generally seen in multiples. They seldom hurt unless pressure is applied to them or when performing weight-bearing activities. Tips to prevent seed corn formation include using a pumice stone to gently file thickened skin, followed by soaking and moisturizing the feet. It can also help to wear shoes and socks that are comfortable and do not rub on the feet. If you have seed corns that are not diminishing, it is suggested that you see a podiatrist for an evaluation and treatment.
If you have any concerns regarding your feet and ankles, contact Brian Shwer, DPM of Southaven Foot Clinic. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Southaven, MS . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.